 It’s a great question.
It’s a great question.
I often state its counter part, “Other people do that and don’t have pain. Let’s work so that you can do that without pain, too.”
Let’s briefly look at few things about trigger points that will answer this question: what they do, their levels of activity, what makes them more active, how we naturally avoid activating them, as well as short and long-term answers for relief.![]()
What trigger points are: They are hyper-irritable spots in muscle with specific behaviors. I’m less interested in the actual spot than most trigger point specialists but here’s an illustration of a trigger point from the most respected researcher in the field.
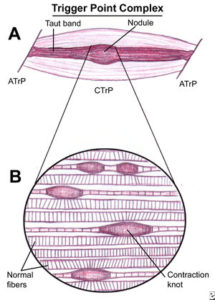 What trigger points do:
What trigger points do:
- They restrict contraction. In many cases, this is that fragile feeling of weakness connected to pain as when a knee buckles walking in stairs or you’re slow to get up or you loose your grip on your coffee cup. Here’s an example in this post.
- They restrict stretch. Obviously, tightness. Even more common is the that we need a minute to get going. It’s when you are slow getting up or stiff for the first few steps.
- They have an associated a referral pattern. It can be more than pain: tingling, “numbing,” itching. Also, there are referral patterns that are not musculoskeletal: inflamed sinuses, blurred vision, irritable bowel, ringing in the ears, fight-or-flight etc. Look at this post.
How common are trigger points? Well, many authors have been able to write about them and research shows that we all have the same trigger points in the same muscles that will generate about the same patterns. Whether or not you feel it is just a matter of how active that particular trigger point is. They are like that app on your phone that reports financial information. It protects you by alarming when you need to restrict your activity or get help.
We refer to trigger points as having 4 levels of activity:
- Level 0 – These are inactive and don’t bother you, even when you press into the muscle or stretch or hike the Grand Tetons. Not every muscle is tender when you press into it, your therapist is just good at finding them.
- Level 1 – These are sensitive and may produce the referral pattern when you press on them. These are pretty common in people’s bodies and largely go unnoticed. This is what makes a client say, “I didn’t know that I hurt there until you pressed on it.”
- Level 2 – These generate some weakness, restriction, pain and other associated referrals when we move. As I said above, trigger points restrict contraction and stretch. These trigger points have become more active and they let you know when you try to do either of those. This is the most common level of activity that I see in my practice and is what I describe in posts like this under the heading “Client’s Description.”
- Level 3 – These continue to generate a referral pattern and bother you, even when you are rest. They make people really miserable as they can’t sleep, sit or work without that constant backache, headache, shoulder pain or whatever the trigger point is generating.
Trigger points become more active for several reasons:
- Something has damaged the muscle like blunt trauma. It generates trigger points to limit contraction and stretch while it is healing. This is why ice and rest are recommended in the first 48 hours after most injuries, not stretching.
- The muscle is protecting a joint that is displaced – I can consistently activate and de-activate trigger points by fixing problems in the associated joints. A big part of my practice is testing to see which muscles aren’t contracting and stretching and then gently working the associated joints to provide lasting relief. It prepares muscle so that direct muscle work is less intense for the client and the relief is longer lasting. When people slip on a rug or get jerked by the dog, joints get displaced and muscles develop trigger points to protect those joints.
- When we have a Level 1 trigger point, we naturally adapt our movement to avoid lengthening and contracting that muscle. We turn a foot out, lean forward when we walk, turn our wrist to pick something up or slide forward in the seat. These adaptations are a natural part of motor planning that we learned as a child when we developed coordination. You can override this natural tendency in a few ways:
- You get chilled – muscles involuntarily contract to generate warmth. I write about that pain in this post.
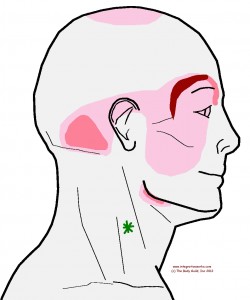
 You are just doing that activity more. This illustration is from a post about a headache around the brow. It is one of the most common trigger points that I treat. It is aggravated by pulling the head forward and to one side while reading. In his case, there’s a mild Level 1 trigger point that becomes more active because the muscle is being used more.
You are just doing that activity more. This illustration is from a post about a headache around the brow. It is one of the most common trigger points that I treat. It is aggravated by pulling the head forward and to one side while reading. In his case, there’s a mild Level 1 trigger point that becomes more active because the muscle is being used more.- Or (drum roll…) You knowingly did something that is unfamiliar that works a muscle with a mildly active trigger point. It wasn’t bothering you. Your body had adapted and was just fine until you decided to weed the flower bed, or throw the ball with your kid, or hike in the beautiful mountain weather. You didn’t notice that it was working differently as you naturally motor planned around it. Muscles that were happily less active are now barking at you because they are being forced to contract and lengthen when they were poised to protect an acquired problem. They have moved from Level 1 to Level 2 or Level 3.
- There are a few other reasons why trigger points become more active. They are less common and fairly tedious to talk about in this post. They include things like raging infection and somatovisceral reflex. Your practitioner is trained to recognize these and refer you to someone who can help.
There are short and long term solutions.
- In the short term, if you are okay with your limited activity, most of my posts offer a stretch that releases the trigger point and may put you back to a Level 1 where you were happily living with limited movement and adaptive motor planning. Ice and stretch is particularly great at this. It quickly and dramatically drops the level of the trigger point’s activity. If the underlying problem was fleeting and your body doesn’t need to restore a higher level of protection, it is a great solution. There are other self-care posts in the menu that help to break up patterns and offer symptomatic relief.
- If you have to participate in a daily self-care routine to stay out of pain, look at a solution that fixes the underlying problems. There are bodywork techniques that create a body that is more self-correcting. I focus on joint work, especially in the craniosacral system. Here’s a post about releasing trigger points in the leg using cranial techniques. Also, I find that structural work, which changes the shape and length of things, produces longer lasting results than functional work, which changes how things coordinate and behave.
These days, catch word is “integrative.” It’s the idea that you fix key parts so that the system works to integrate itself. Identifying trigger points is a good start. Your bodyworker may be a chiropractor, neuromuscular therapist, osteopath, or physical therapist but finding one that does integrative work is the long-term solution.
If you’re a practitioner, you might enjoy this more technical paper on trigger point concepts.
![]() Tony Preston has written and taught about anatomy, trigger points and cranial therapies since the mid-90s. He has a practice in Atlanta, Georgia where he sees clients.
Tony Preston has written and taught about anatomy, trigger points and cranial therapies since the mid-90s. He has a practice in Atlanta, Georgia where he sees clients.
Question? Comment? Want a session with Tony?
The Body Guild.org
(404) 226-1363
tony@thebodyguild.org


 You are just doing that activity more. This illustration is from a post about a headache around the brow. It is one of the most common trigger points that I treat. It is aggravated by pulling the head forward and to one side while reading. In his case, there’s a mild Level 1 trigger point that becomes more active because the muscle is being used more.
You are just doing that activity more. This illustration is from a post about a headache around the brow. It is one of the most common trigger points that I treat. It is aggravated by pulling the head forward and to one side while reading. In his case, there’s a mild Level 1 trigger point that becomes more active because the muscle is being used more.