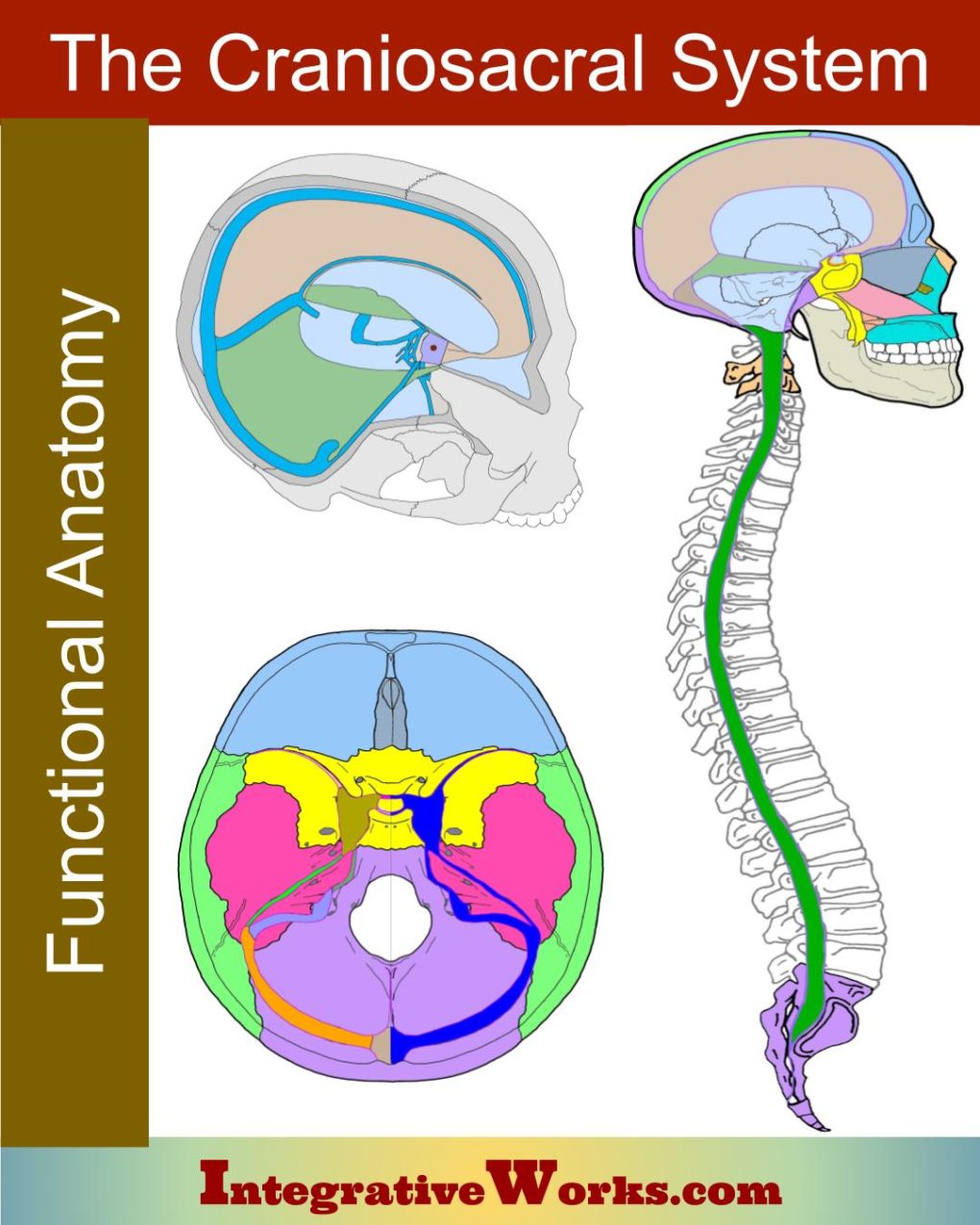
Osteopathic BioMechanical Model
This post on The Osteopathic Biomechanical approach is part of a collection of posts on craniosacral.
This collection includes posts about history, treatment models, techniques, concepts, and cases.
Osteopathic Cranial Arrives

The Founder
In every field, there are visionaries. And then, there is that one person who moves the vision forward by developing credibility. And who then takes the necessary risks to innovate.
In the 1800s, there were innovators called “bone-setters.” They eventually split into two groups. The chiropractors followed Daniel David Palmer into a discipline without drugs and surgery. Osteopaths followed Andrew Taylor Still into a discipline that embraced allied medicine.
After many years of study and experimentation, Still gave birth to osteopathic science in 1874. 35 years later, he published Osteopathy: Research and Practice, confirming the principles of his earlier assertion. He also took risks and made innovations. Rightfully, he is revered for his persistence, insight, principles, and accomplishments.
Like Rollin Becker and Robert C. Fulford, many legendary practitioners write of Still’s visionary accomplishments in cranial osteopathy. Also, he opened the door and created the playing field for Sutherland.

The Visionary
William Garner Southerland was the innovator who humbly persevered to establish craniosacral as a credible treatment approach. Almost every model of craniosacral treatment reveres his accomplishments. He overcame great controversy and opposition. I’ve gathered a few notes on his life in this post. Again, he persevered, took risks, and innovated.
In the beginning, Sutherland spent more than twenty years defining the structure and movement of each bone in the craniosacral system. He spent another ten years defining the fluid flow dynamics of the system. He developed what is known as the “osteopathic model.”
The great text from his teaching foundation is Osteopathy in the Cranial Field by Harold Ives Magoun. It demonstrates how every piece of anatomy has a structural and functional role in the model. The bones flex and protect, as do the membranes. Fluid supports, cushions, and nourishes. The ventricles create cerebrospinal fluid (CSF) and support the neural tissue of the brain.
The motility of each bone and the mobility of each joint is explained in detail as well. And, the text covers the assessment and treatment of the system. We can admire that Magoun’s book presents a detailed model before technology was available to facilitate that study.
His concept, from the beginning, focused on what he called “Primary Respiration.” He noted that the wings of the sphenoid bone look like the gills of a fish. As a result, he would interpret this system’s motility as “inhaling” and “exhaling.” The concepts behind this motility are a little different between the biomechanical model and the biodynamic model.
Sutherland’s Principles
Although texts vary somewhat on this list, authors suggest five principles or components in Sutherland’s craniosacral approach:
- The articular mobility of cranial bones.
- Mobility of the cranial and spinal dural membranes.
- The inherent mobility of the central nervous system.
- Involuntary mobility of the sacrum between the ilia.
- The fluctuation of cerebrospinal fluid.
These principles permeate most approaches to craniosacral treatment, even the approaches that focus on the subtle energies. Variations on this list include a version of the holistic model or the body’s ability to heal when restrictions are removed.
If you don’t know much about the craniosacral system’s anatomy, take a look at this simplified understanding of the craniosacral system. It is short, easy to read, and will make the rest of this more understandable.
Primary Respiration, The Tide, Breath of Life, craniosacral impulses, the craniosacral cycle, and craniosacral rhythm refer to the fluctuation of fluid associated with craniosacral motility. For the seasoned practitioner, they reference important differences in the concepts.
The BioMechanical Model
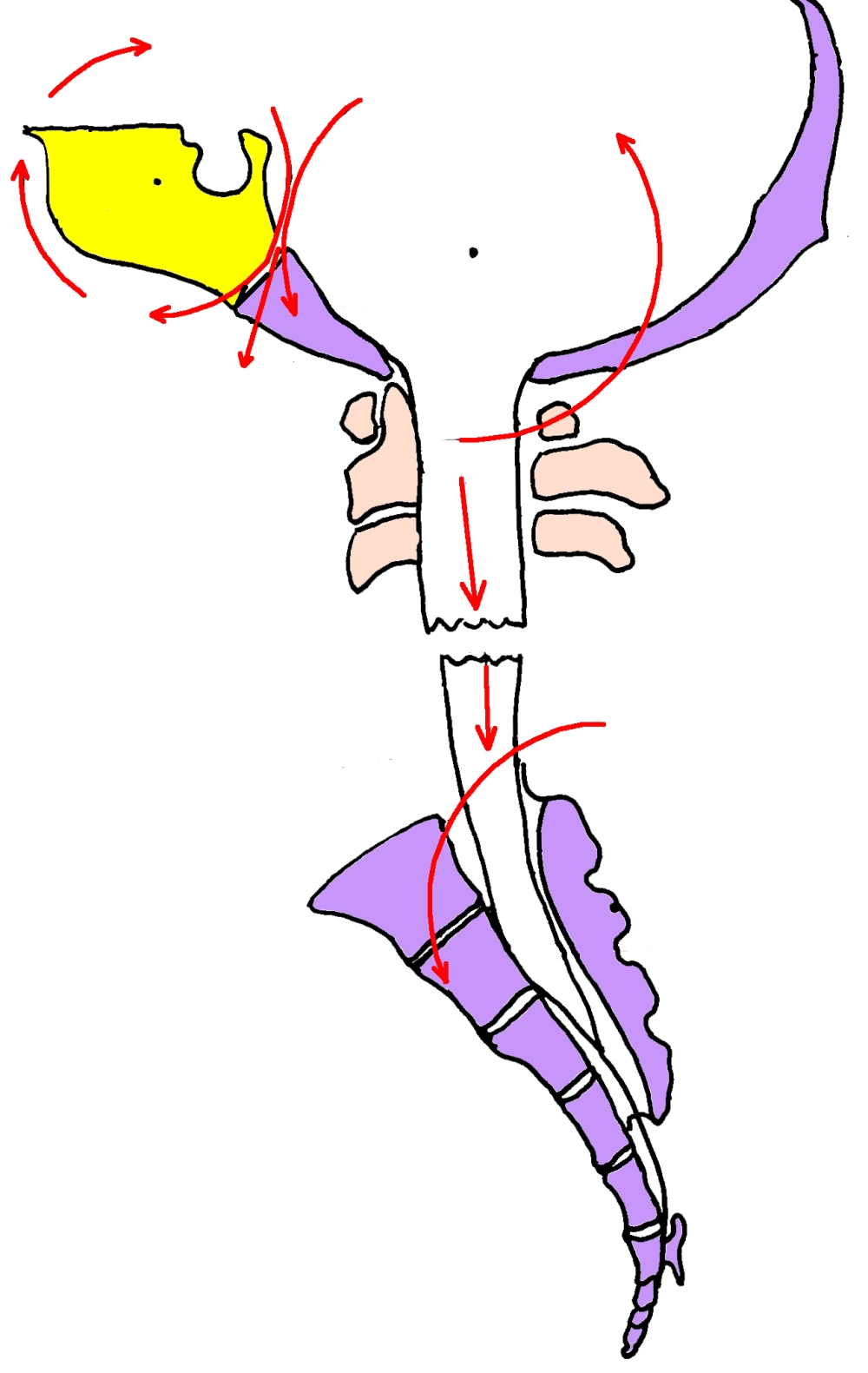
This osteopathic model is a biomechanical model. It defines a very physically-based system. Mechanically, it is a semi-closed hydraulic system. Fluid pressure fluctuates as it is inhaled and exhaled. This tide of fluid and the motion that it creates are central to the craniosacral concept. Focus on this rhythmic wave separates craniosacral techniques from other forms of cranial treatments.
Primary Respiration in the Biomechanical Model
The biomechanical model is based on flexion and extension of the sphenobasilar mechanism, as it is associated with CSF circulation.
Cerebrospinal fluid (CSF) is filtered from the blood and fills the ventricles. Then, it leaks into the subarachnoid space between the central nervous system and bones. Next, it washes over the pia mater of the brain and spinal cord. The building pressure rotates bones and stretches reciprocal tension membranes. On exit, valves open to allow the CSF to empty into sleeves called venous sinuses. These sinuses run between layers of the meninges. At the base of the cranium, blood, rich with CSF, returns to circulation through the jugular vein.
Therapeutic Approach in the BioMechanical Model
In this model, the practitioner identifies restrictions, imbalances, or what the osteopaths refer to as “lesions.” In general, they work to balance motion and increase the amplitude of cerebrospinal fluid flow. On the other hand, there are quite specific techniques for conditions such as restricted breathing, sinus congestion, or stiff neck.
The assessment methods, the pressure used, and objectives vary from one approach to another. On the whole, contact tends to be very gentle, and movements are slow. Techniques tend to decompress, release, and unwind connective tissues. There is a focus on the flexibility of bone and remodeling those structures.
Some techniques target restrictions in specific membranes, blood vessels, or nerves. Other techniques decompress the larger structure. Often, protocols focus a sequence of techniques on a larger objective like draining the venous sinuses or freeing restrictions along a nerve path. Other protocols systematically balance the entire structure.
This explanation of techniques may seem a bit generic and vague. It is because innovators have done a lot with the foundations that Sutherland has built. I’ll discuss those innovations as I explore other models.
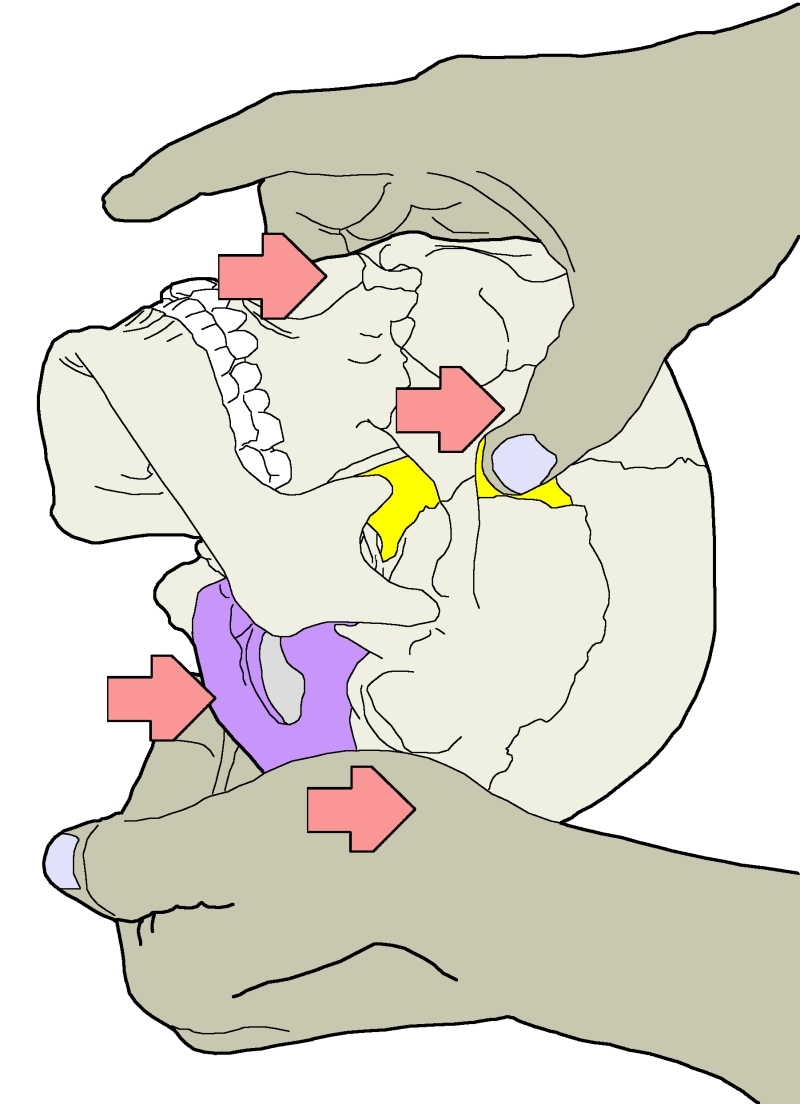
My Experience in the Biomechanical Model
My initial exploration of craniosacral work was with the craniostructural techniques of Dallas Hancock, DC. He, like myself, was a software engineer before getting into bodywork. It was natural and easy to explore the craniosacral mechanism through structure and associated function with him.
Craniostructural techniques are strongly rooted in biomechanical craniosacral. This approach focuses on the axes of movement, specific rotation of bones during the cycle, and the pivots and bevels that make it possible. Compare this illustration of initiating craniosacral extension with the diagram of axes of motion in the previous section. Illustrations like these allow you to see the biomechanics more simply.
I taught this work for the National Institute of Craniosacral Studies in the 90s. Later, I created my own teaching for Integrative Craniosacral. I have detailed this work in text and illustrations like those in this post for more than 25 years.
Biomechanical craniosacral has been a reliable vehicle for my practice as well. Among other things, I employ it to:
- assess and treat craniosacral restrictions
- address trigger point pain in the body
- release neurovascular restrictions
- balance chakras and meridians
- regulate special needs children
- facilitate Integrative Modulation in adults
Support Integrative Works to
stay independent
and produce great content.
You can subscribe to our community on Patreon. You will get links to free content and access to exclusive content not seen on this site. In addition, we will be posting anatomy illustrations, treatment notes, and sections from our manuals not found on this site. Thank you so much for being so supportive.
Cranio Cradle Cup
This mug has classic, colorful illustrations of the craniosacral system and vault hold #3. It makes a great gift and conversation piece.
Tony Preston has a practice in Atlanta, Georgia, where he sees clients. He has written materials and instructed classes since the mid-90s. This includes anatomy, trigger points, cranial, and neuromuscular.
Question? Comment? Typo?
integrativeworks@gmail.com
Interested in a session with Tony?
Call 404-226-1363
Follow us on Instagram

*This site is undergoing significant changes. We are reformatting and expanding the posts to make them easier to read. The result will also be more accessible and include more patterns with better self-care. Meanwhile, there may be formatting, content presentation, and readability inconsistencies. Until we get older posts updated, please excuse our mess.